The inflammatory eye disorder autoimmune uveitis occurs when a person's immune system goes awry, attacking proteins in the eye. What spurs this response is a mystery, but now a study on mice suggests that bacteria in the gut may provide a kind of training ground for immune cells to attack the eye. The study was conducted by researchers at the National Eye Institute (NEI), part of the National Institutes of Health.
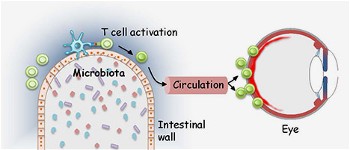
Microbiota in the gut activate T cells that are able to recognize retinal proteins. These activated T cells then migrate through the bloodstream to the eye, where they cause the inflammatory response associated with autoimmune uveitis.
Evidence increasingly suggests that there is an association between the microbiota in the gut - bacteria, fungi and viruses - and the development of autoimmune disorders. Findings from this study suggest how that association may be made and therefore have implications about the origins of autoimmune diseases not only in the eye, but also elsewhere in the body, said Rachel R. Caspi, Ph.D., a senior investigator at NEI whose lab led the study.
Autoimmune uveitis accounts for more than 10 percent of severe visual disability in the United States. Corticosteroids provide a blanket approach to the disorder by quelling inflammation, but their long-term use can lead to adverse side effects.
Understanding what spurs autoimmune uveitis is fundamental to the development of safer long-term therapies and possibly even strategies for preventing it, said Reiko Horai, Ph.D., a staff scientist at NEI and a lead author of the study, published in the journal Immunity. Carlos R. Zarate-Blades, Ph.D., a postdoctoral fellow at NEI, is the other lead author.
The eye is one of the places in the body that has immune privilege meaning it is protected by a blood-tissue barrier that physically separates it from the rest of the body and minimizes the exchange of substances and blood-borne cells going in and out of the eye.
In the case of autoimmune uveitis, immune cells (T cells) are thought to penetrate through
this blood-ocular barrier. But first, they must become activated, which occurs when they come in contact with the protein that they are pre-programmed to recognize. This is how T cells fight an infection and some types of cancer - by targeting proteins on bacteria, viruses and cells. And herein lies a paradox that's been puzzling uveitis researchers. The proteins believed to be targeted in autoimmune uveitis are sequestered in the eye; they don't exist elsewhere in the body. So what activates the T cells and allows them to cross the blood-ocular barrier?
The researchers asked this question by studying mice genetically engineered to develop autoimmune uveitis, due to a high level of retina-reactive T cells in their bodies. Before the mice had developed signs of the disease, the team searched their bodies for activated T cells and made an interesting discovery. Levels of activated T cells were not elevated in the lymph nodes (the glands that tend to swell during infections), but they were abundant in the intestines. What's more, the T cells in the gut produced a protein shown in previous studies by Dr. Caspi's team to augment the damage in autoimmune uveitis.
"These discoveries support the idea that activation of T cells in the gut may actually precede the first signs of the disease," she said. To test that idea, the researchers gave the mice an antibiotic cocktail designed to wipe out a broad spectrum of bacteria in the gut and by rearing them in a germ-free environment. They found that mice without gut bacteria developed autoimmune uveitis much later, and with less severity, compared to control mice with normal gut flora.
There was a similar delay in uveitis and decline in its severity when the uveitis-prone mice were raised in an environment free of bacteria and other germs. But when the same mice were later moved into normal housing, where they acquired normal gut bacteria, the uveitis roared in at full strength.
So how do bacteria in the gut activate T cells against cells in the eye? The researchers theorize that bacteria in the gut produce a molecule that, to T cells, looks similar to a protein in the retina. This gives the T cells marching orders to look for that retinal protein and attack it. Consistent with this idea, the researchers found that they could activate retina-specific T cells by exposing them to a soup of bacterial proteins extracted from mouse intestines. When those activated T cells were injected into normal mice (not prone to uveitis), the mice developed uveitis.
"Given the huge variety of bacteria in our intestines, if they can mimic a retinal protein, it is conceivable that they could also mimic other self-proteins in the body. So we believe that normally harmless bacteria in the gut could be involved in promoting other autoimmune diseases as well," Dr. Caspi said.
The results don't have immediate implications for patients, but will help inform further research to understand the disease and help to develop new therapies, Dr. Caspi said. Eliminating bacteria from our bodies isn't a treatment option, and a bacteria-free state would not be feasible. However, if scientists could one day identify the bacteria specifically involved in promoting autoimmune uveitis, it might be possible to target only those of interest.
NEI leads the federal government's research on the visual system and eye diseases. NEI supports basic and clinical science programs that result in the development of sight-saving treatments. For more information, visit
http://www.nei.nih.gov.















 1
1 2
2 3
3 4
4 5
5 this blood-ocular barrier. But first, they must become activated, which occurs when they come in contact with the protein that they are pre-programmed to recognize. This is how T cells fight an infection and some types of cancer - by targeting proteins on bacteria, viruses and cells. And herein lies a paradox that's been puzzling uveitis researchers. The proteins believed to be targeted in autoimmune uveitis are sequestered in the eye; they don't exist elsewhere in the body. So what activates the T cells and allows them to cross the blood-ocular barrier?
this blood-ocular barrier. But first, they must become activated, which occurs when they come in contact with the protein that they are pre-programmed to recognize. This is how T cells fight an infection and some types of cancer - by targeting proteins on bacteria, viruses and cells. And herein lies a paradox that's been puzzling uveitis researchers. The proteins believed to be targeted in autoimmune uveitis are sequestered in the eye; they don't exist elsewhere in the body. So what activates the T cells and allows them to cross the blood-ocular barrier?





